Metabolic–Renal Divergence in Diabetic Patients Three Months After COVID-19: Evidence from a Real-World Cohort
DOI:
https://doi.org/10.54133/ajms.v10i2.2814Keywords:
COVID-19, Cohort study, Diabetes mellitus, Glycemic control , Renal function , Therapeutic inertiaAbstract
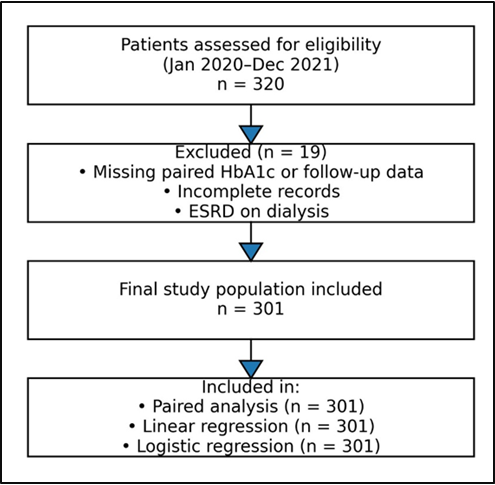
Background: The short-term impacts of COVID-19 in diabetes are still unknown as well. When glycemic improvement is followed by renal stabilization in a patient after treatment of COVID-19 infection. Objective: To evaluate three-month glycemic and renal trajectories following COVID-19 infection and to identify predictors of persistent poor glycemic control. Methods: This retrospective real-world cohort study included 301 adults with diabetes and confirmed COVID-19 infection. Baseline measurements were obtained at the first post-COVID clinical assessment, and follow-up measurements were recorded approximately three months later. Paired t-tests assessed within-subject changes in HbA1c, fasting plasma glucose (FPG), and serum creatinine. McNemar’s test evaluated shifts in glycemic control category (HbA1c<8%). Multivariable linear and logistic regression analyses identified predictors of glycemic change and persistent poor control. Effect sizes were calculated using Cohen’s d. Results: HbA1c was significantly decreased (9.08±2.22% to 8.43±2.04%. FPG was reduced (51 mg/dL; p < 0.001). The creatinine level remained similarly in line but slightly rose in diabetic patients at 3 months of chronic comorbidity (+ 0.094mg/dL; p=0.001), an indication of metabolic-renal divergence. Significant improvement of the glycemic control category was observed as well (p<0.001). Conclusion: Three months after COVID-19 treatment, there was a positive correlation between glycemic control and glucose decline, along with a reasonable renal outcome. This clearly illustrates an acute need for early cardiometabolic care after infection.
Downloads
References
International Diabetes Federation. Global diabetes burden 2024 report. Diabetes Res Clin Pract. 2024;201:110678. doi: 10.1016/j.diabres.2024.110678.
Pal R, Banerjee M. COVID-19 and glycemic control: longitudinal outcomes in diabetes. Front Endocrinol (Lausanne). 2023;14:1187432. doi: 10.3389/fendo.2023.1187432.
McCrimmon RJ, Das AK. Glycemic variability and outcomes in COVID-19. Diabetes Res Clin Pract. 2024;210:110465. doi: 10.1016/j.diabres.2024.110465.
Li J, Huang DQ, Zou B, Yang H, Hui WZ, Rui F, et al. Epidemiology of long COVID and metabolic consequences. BMJ. 2023;381:e072452. doi: 10.1136/bmj-2022-072452.
Khunti K, Gomes MB, Pocock S, Shestakova MV, Pintat S, Fenici P, et al. Therapeutic inertia in diabetes care: 2023 update. Diabetes Obes Metab. 2023;25(4):937–949. doi: 10.1111/dom.14942. DOI: https://doi.org/10.1111/dom.14942
Son JW, Lee YH, Kim YG, Park CY, Kim DJ, Lee BW, et al. Therapeutic inertia and diabetes outcomes. J Clin Endocrinol Metab. 2024;109(3):e927–e936. doi: 10.1210/clinem/dgad821.
Qin YY, Zhu L, Cai J, Liu Y, Chen Z, Wang X, et al. Post-COVID-19 renal outcomes. Nephrol Dial Transplant. 2024;39(7):1115–1127. doi: 10.1093/ndt/gfad059. DOI: https://doi.org/10.1093/ndt/gfad059
Greenwood SA, Oliveira BA, Asgari E, Ayis S, Baker LA, Beckley-Hoelscher N, et al. A randomized trial of intravenous iron supplementation and exercise on exercise capacity in iron-deficient nonanemic patients with CKD. Kidney Int Rep. 2023;8(8):1496-1505. doi: 10.1016/j.ekir.2023.05.002. DOI: https://doi.org/10.1016/j.ekir.2023.05.002
Agarwal R, Gansevoort RT, Rizk DV, Levin A, Pecoits-Filho R, Levey AS, et al. Chronic kidney disease after COVID-19. Kidney Int. 2023;104(1):7–19. doi: 10.1016/j.kint.2023.02.012 DOI: https://doi.org/10.1016/j.kint.2023.02.012
American Diabetes Association Professional Practice Committee. Standards of care in diabetes—2024. Diabetes Care. 2024;47(Suppl 1):S1–S350. doi: 10.2337/dc24-Sint. DOI: https://doi.org/10.2337/dc24-SINT
Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA, Adler AI. Impact of HbA1c reduction on microvascular outcomes. Diabetologia. 2023;66(6):987–995. doi: 10.1007/s00125-023-05834-2.
McCoy RG, Van Houten HK, Ziegenfuss JY, Shah ND, Wermers RA, Smith SA. Clinical inertia in diabetes. Mayo Clin Proc. 2023;98(5):913–925. doi: 10.1016/j.mayocp.2023.01.021. DOI: https://doi.org/10.1016/j.mayocp.2023.01.021
Gupta A, Kark JD, Shochat T, Tzur D, Afek A, Grossman E, et al. Hypertension and diabetes: integrative risk management. J Clin Hypertens. 2024;26(5):487–496. doi: 10.1111/jch.14678. DOI: https://doi.org/10.1111/jch.14678
Wu J, Zhang P, Yang X, Liu Y, Chen H, Li Z, et al. Impact of hypertension on glycemic outcomes. Am J Hypertens. 2023;36(11):990–999. doi: 10.1093/ajh/hpad082. DOI: https://doi.org/10.1093/ajh/hpad082
Sterling KL, Shapiro BP, Cooper-DeHoff RM, Carter BL, Calhoun DA, Bakris GL. RAAS blockade and metabolic modulation. Curr Diab Rep. 2023;23(12):600–614. doi: 10.1007/s11892-023-01534-2.
Al-Aly Z, Bowe B, Xie Y. Post-acute COVID organ sequelae. Nat Med. 2024;30(1):35–45. doi: 10.1038/s41591-023-02618-6.
Banerjee S, Sulaiman R, Hussain N, Ahmed A, Patel K, Sharma R, et al. Clinical pharmacy interventions reduce therapeutic inertia. Diabetes Ther. 2025;16(4):985–1001. doi: 10.1007/s13300-025-01560-1.
Pantalone KM, Hobbs TM, Wells BJ, Kong SX, Kattan MW, Bouchard J, et al. Real-world therapeutic inertia and glycemic outcomes. Diabetes Ther. 2023;14(7):1385–1398. doi: 10.1007/s13300-023-01402-3.
Pugliese G, Solini A, Bonora E, Ceriello A, Mannucci E, Monami M, et al. Integrated cardiometabolic care in diabetes. Nat Rev Endocrinol. 2025;21(1):12–30. doi: 10.1038/s41574-024-00823-4.
Bornstein SR, Rubino F, Khunti K, Mingrone G, Hopkins D, Birkenfeld AL, et al. Management of diabetes in the context of COVID-19. Lancet Diabetes Endocrinol. 2024;12(3):176–188. doi: 10.1016/S2213-8587(23)00284-6.
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 )

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Published by Al-Rafidain University College. This is an open access journal issued under the CC BY-NC-SA 4.0 license (https://creativecommons.org/licenses/by-nc-sa/4.0/).











