Systemic Immune-Inflammation Index and Hematological Ratios as Indicators of Hepatic Dysfunction in Thalassemia-Associated Liver Disease
DOI:
https://doi.org/10.54133/ajms.v10i2.2883Keywords:
Liver disease, Neutrophil-to-lymphocyte ratio, Prothrombin time , Systemic inflammation, Systemic immune-inflammation index, ThalassemiaAbstract
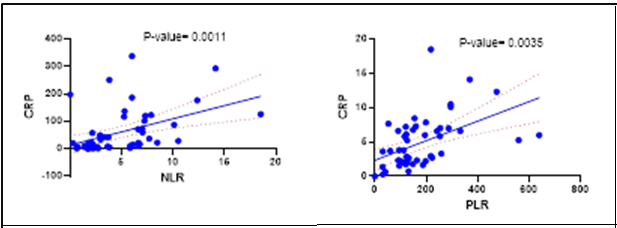
Objective: This study aimed to investigate the relationship between systemic inflammatory biomarkers and clinical and biochemical indicators of liver dysfunction in patients with thalassemia-associated liver disease. Methods: A cross-sectional study was conducted involving 50 patients with thalassemia-associated liver disease. Demographic characteristics, hematological parameters, inflammatory biomarkers, and liver function tests were collected. Inflammatory indices including neutrophil-to-lymphocyte ratio (NLR), platelet-to-lymphocyte ratio (PLR), lymphocyte-to-monocyte ratio (LMR), and systemic immune-inflammation index (SII) were calculated from routine complete blood count parameters. Pearson correlation analysis was performed to evaluate associations between inflammatory biomarkers and indicators of hepatic dysfunction, including prothrombin time (PT) and international normalized ratio (INR). Multivariate regression analysis was applied to identify independent predictors of symptom burden. Results: The mean age of participants was 52.1±19.7 years, with a predominance of female patients. C-reactive protein (CRP) showed significant positive correlations with NLR (r=0.45, p=0.001), PLR (r=0.41, p=0.003), and SII (r=0.50, p<0.001) and a significant inverse correlation with LMR (r=−0.50, p<0.001). NLR exhibited a strong correlation with SII (r=0.91, p<0.0001). However, leukocyte-derived indices were not significantly associated with PT or INR. Both PT and INR correlated significantly with CRP and LMR. Multivariate analysis identified PT as the only independent predictor of symptom burden (p<0.0001). Conclusions: Inflammatory biomarkers reflect systemic immune activation in thalassemia-associated liver disease, whereas PT remains the most reliable indicator of disease severity. Integrating inflammatory indices with conventional liver function markers may improve clinical assessment.
Downloads
References
Thalassemia International Federation. Guidelines for the Management of Transfusion Dependent Thalassemia, (3rd Edition), (2014) Accessed: March, 2026. Available at: https://thalassaemia.org.cy/download/guidelines-for-the-management-of-transfusion-dependent-thalassaemia-3rd-edition-2014-english/
Taher AT, Musallam KM, Cappellini MD. β-Thalassemias. N Engl J Med. 2021;384(8):727-743. doi: 10.1056/NEJMra2021838. DOI: https://doi.org/10.1056/NEJMra2021838
Porter JB, Garbowski M. The pathophysiology of transfusional iron overload. Hematol Oncol Clin North Am. 2014;28(4):683-701. doi: 10.1016/j.hoc.2014.04.003. DOI: https://doi.org/10.1016/j.hoc.2014.04.003
Nemeth E, Ganz T. Hepcidin and iron in health and disease. Annu Rev Med. 2023 ;74:261-277. doi: 10.1146/annurev-med-043021-032816. DOI: https://doi.org/10.1146/annurev-med-043021-032816
Qiu X, Shen S, Jiang N, Feng Y, Yang G, Lu D. Associations between systemic inflammatory biomarkers and metabolic dysfunction associated steatotic liver disease: a cross-sectional study of NHANES 2017-2020. BMC Gastroenterol. 2025;25(1):42. doi: 10.1186/s12876-025-03625-4. DOI: https://doi.org/10.1186/s12876-025-03625-4
Xue B, Wang Z, Li J. Systemic immune-inflammation index as a prognostic marker for chronic Hepatitis B with non-alcoholic fatty liver disease. J Infect Dev Ctries. 2025;19(2):315-324. doi: 10.3855/jidc.19636. DOI: https://doi.org/10.3855/jidc.19636
Liu K, Tang S, Liu C, Ma J, Cao X, Yang X, et al. Systemic immune-inflammatory biomarkers (SII, NLR, PLR and LMR) linked to non-alcoholic fatty liver disease risk. Front Immunol. 2024;15:1337241. doi: 10.3389/fimmu.2024.1337241. DOI: https://doi.org/10.3389/fimmu.2024.1337241
Ma Y, Wang J, Du L, Tang H. Association between the systemic immune-inflammation index and the outcome of liver fibrosis in patients with chronic hepatitis C. Front Med (Lausanne). 2024;11:1486503. doi: 10.3389/fmed.2024.1486503. DOI: https://doi.org/10.3389/fmed.2024.1486503
Kadhim RGH, Hassan MH, Ghatheth SFS, Ahmed AKJ. A comprehensive chemical and laboratory assessment of blood plasma in evaluating liver and kidney functional disorders. 2025;9(12):1283–1291. doi: 10.33545/26174693.2025.v9.i12p.6796. DOI: https://doi.org/10.33545/26174693.2025.v9.i12p.6796
Agarwal M, Cottam S. Laboratory tests in hepatic failure. Anaesth Intens Care Med. 2009;10(7):326–327. doi: 10.1016/J.MPAIC.2009.04.006. DOI: https://doi.org/10.1016/j.mpaic.2009.04.006
Yang R, Zubair M, Moosavi L, (Eds.), Prothrombin Time, Transfusion Medicine and Hemostasis: Clinical and Laboratory Aspects, Jan. 2024, pp. 659–662. doi: 10.1016/B978-0-323-96014-4.00022-7. DOI: https://doi.org/10.1016/B978-0-323-96014-4.00022-7
Rasheed RH, Aziz TA. Cardioprotective effects of SAR through attenuating cardiac-specific markers, inflammatory markers, oxidative stress, and anxiety in rats challenged with 5-fluorouracil. J Xenobiot. 2025;15(4):130. doi: 10.3390/jox15040130. DOI: https://doi.org/10.3390/jox15040130
Rafiq SB, Aziz TA, Nuradeen BE, Salh HJH, Hussain SA, Preliminary evaluation of tacrolimus impact on glycemic control, renal function, and hematological inflammatory markers in kidney transplant recipients. Al-Rafidain J Med Sci. 2025;9(2):114–121. doi: 10.54133/AJMS.V9I2.2392. DOI: https://doi.org/10.54133/ajms.v9i2.2392
Baiz HQ, Ibrahim AI, Othman HH, Ali PG, Aziz TA, Ahmed ZA. Molecular docking-guided experimental evaluation of Azilsartan gel as therapeutic potential in a rat burn model. J Renin-Angiotensin-Aldosterone Syst. 2025;26. doi: 10.1177/14703203251386321. DOI: https://doi.org/10.1177/14703203251386321
Pepys MB, Hirschfield GM. C-reactive protein: a critical update. J Clin Invest. 2003;111(12):1805-1812. doi: 10.1172/JCI18921. DOI: https://doi.org/10.1172/JCI200318921
Sproston NR, Ashworth JJ. Role of C-reactive protein at sites of inflammation and infection. Front Immunol. 2018;9:754. doi: 10.3389/fimmu.2018.00754. DOI: https://doi.org/10.3389/fimmu.2018.00754
Laleman W, Claria J, Van der Merwe S, Moreau R, Trebicka J. Systemic inflammation and acute-on-chronic liver failure: Too much, not enough. Can J Gastroenterol Hepatol. 2018;2018:1027152. doi: 10.1155/2018/1027152. DOI: https://doi.org/10.1155/2018/1027152
Cai XH, Tang YM, Chen SR, Pang JH, Chong YT, Cao H, et al. Prognostic value of neutrophil-to-lymphocyte ratio in end-stage liver disease: A meta-analysis. World J Hepatol. 2024;16(3):477-489. doi: 10.4254/wjh.v16.i3.477. DOI: https://doi.org/10.4254/wjh.v16.i3.477
Terasaki F, Sugiura T, Okamura Y, Ito T, Yamamoto Y, Ashida R, et al. Systemic immune-inflammation index as a prognostic marker for distal cholangiocarcinoma. Surg Today. 2021;51(10):1602-1609. doi: 10.1007/s00595-021-02312-7. DOI: https://doi.org/10.1007/s00595-021-02312-7
Tripodi A, Mannucci PM. The coagulopathy of chronic liver disease. N Engl J Med. 2011;365(2):147-156. doi: 10.1056/NEJMra1011170. DOI: https://doi.org/10.1056/NEJMra1011170
Tacke F, Zimmermann HW. Macrophage heterogeneity in liver injury and fibrosis. J Hepatol. 2014;60(5):1090-1096. doi: 10.1016/j.jhep.2013.12.025. DOI: https://doi.org/10.1016/j.jhep.2013.12.025
Wu H. European association for the study of the liver (EASL) congress 2024. Lancet Reg Health Eur. 2024;43:100980. doi: 10.1016/j.lanepe.2024.100980. DOI: https://doi.org/10.1016/j.lanepe.2024.100980
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2026 Al-Rafidain Journal of Medical Sciences ( ISSN 2789-3219 )

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.
Published by Al-Rafidain University College. This is an open access journal issued under the CC BY-NC-SA 4.0 license (https://creativecommons.org/licenses/by-nc-sa/4.0/).











